
Calcium and Heart Disease
A new study adds to the increasing data that taking supplements are not always the best way to obtain micronutrients.
A study published in the British Medical Journal, Heart, showed people with increased dietary calcium (not supplements) had a lower risk of heart attack. They looked at 24,000 people between 35 and 64 found that people who had a moderate amount of calcium in their diet had a 31% lower risk of having a heart attack than those who had low levels of calcium in their diet. However, those who took calcium supplements did not have a lower risk of heart attack – in fact had a higher risk of heart disease. To quote from their abstract:
In comparison with non-users of any supplements, users of calcium supplements had a statistically significantly increased MI risk (HR=1.86; 95% CI 1.17 to 2.96), which was more pronounced for calcium supplement only users (HR=2.39; 95% CI 1.12 to 5.12).
You can read the online version here.
Over the last few years there have been increasing number of studies showing that supplements, be they vitamins, minerals, or anti-oxidants, not only show no benefit in terms of preventing heart disease or cancer, but, contrary to popular thinking, people who take supplements might be worse off than those who don’t.
Antioxidants thinking has changed. Recently the USDA removed the ORAC Database for Foods from its website. This chart listed the ORAC values of foods which was maintained by USDA’s Nutrient Data Laboratory. The reason was the mounting evidence that what happens in a test tube does not equal what happens to people. To quote: ”The data for antioxidant capacity of foods generated by in vitro (test-tube) methods cannot be extrapolated to in vivo (human) effects and the clinical trials to test benefits of dietary antioxidants have produced mixed results. We know now that antioxidant molecules in food have a wide range of functions, many of which are unrelated to the ability to absorb free radicals.”
What no one denies is that getting micronutrients from food is far better than supplements. We don’t know why, yet- but it appears purifying the product isn’t always the answer. This is in contrast to medications, where the active ingredient is purified, then tested for toxicity and efficacy, then tested against other agents. Part of the issue is that since the FDA does not regulate supplements and vitamins, they also don’t test them- both for purity or keep track of long-term consequences.
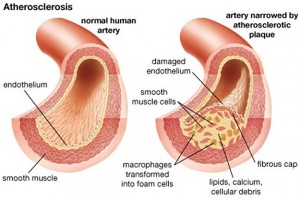
Part of the issue with calcium is a simplistic assumption about arteries. Since arteries clog, chemists have analyzed what they have been clogged with and concluding we should avoid that in the diet. Cholesterol being the first of these to be erroneously blamed for heart disease. As the artery damaged artery ages, calcium is deposited on the wall. There are other diseases where abnormal deposition of calcium becomes pathologic, thus some scientists made the conclusion that more calcium is a cause of atherosclerosis. There have been multiple studies with conflicting results about with calcium and heart disease – this being the first to separate calcium in the diet from calcium supplementation.
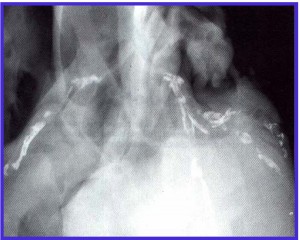
Some arteries are so calcified you can see them on a regular x-ray. The white arteries on the right of this photo are the coronary arteries of the heart
Does this say you should not take supplements? No – not quite yet. But it points out the need to have a balanced diet- make certain to have enough calcium in your diet. There are those who need calcium supplementation, such as those who have had long-limb malabsorptive weight loss procedures, duodenal switch and the RNY bypass, who need additional calcium supplementation, or others who need oral calcium supplement to avoid kidney stones.
For those who have lactose intolerance and cannot take dairy, or those who won’t take dairy products, Kale, and other vegetables makes a great source for these, and you might consider adding this to a regimen (shake recipes here).
REFERENCES:
Heart 2012;98:920-925 doi:10.1136/heartjnl-2011-301345. Calcium and cardiovascular disease Associations of dietary calcium intake and calcium supplementation with myocardial infarction and stroke risk and overall cardiovascular mortality in the Heidelberg cohort of the European Prospective Investigation into Cancer and Nutrition study (EPIC-Heidelberg). Am J Med. 2012 Apr;125(4):e15; author reply e17.
Calcium supplements and risk of myocardial infarction: an hypothesis twice tested.. Reid IR, Bolland MJ, Grey A.
Antioxidant supplements for prevention of mortality in healthy participants and patients with various diseases. Goran Bjelakovic1,Dimitrinka Nikolova, Lise Lotte Gluud, Rosa G Simonetti, Christian Gluud
