
President Eisenhower followed a low-cholesterol diet with military precision. But his cholesterol continued to climb. Even with exercise and strictly eating no foods with fat. He listened to the best medical advice of the day- and they were wrong.
In Gary Taubs book he will relate the following stories to show that our view of dietary cholesterol was incorrect. He will point out that President Eisenhower could not have been more frustrated. Following the advice of his cardiologist and General Thomas Mattingly, and the famed Paul Dudley White, Eisenhower was eliminating all cholesterol and fat from his diet. But every time they would take his blood level his cholesterol was higher. He was no stranger to exercise, he gave up smoking in 1949, and days he would just have grapefruit with some melba toast. The blood cholesterol would come back, higher than before. It was so frustrating that the White House physicians seeing him would make up numbers to tell him that it was getting better. But it didn’t. Eisenhower was crippled in retirement by his heart disease – determined to eat as prescribed, he ended his days as a cardiac cripple.
Taubs will point out that Lyndon B Johnson had a heart attack while he was a senator. General Thomas Mattingly was also his physician. Mattingly prescribed the same low fat diet that he had given to President Eisenhower. For months after his first attack Johnson followed it to the letter, shedding some 4o pounds and feeling better. But still his cholesterol was high.

LBJ, a heart patient, tried the “low cholesterol, low fat” diet, but realized his cholesterol didn’t change – so he gave it up. Remarkably, once he started eating the beef from his ranch his cholesterol decreased.
Johnson fell back into his old habits, and had another heart attack, which derailed his presidential ambitions for a while. He came to his own conclusions, stopped trying to avoid beef- and enjoyed the bounties of his retirement. He enjoyed friends coming to the ranch, with frequent barbecues – often coming late for dinner.
For years America was told saturated fat is bad for your heart. It was based on a faulty principle – that the fat in the arteries came from the fat in the blood which came from the fat in the diet. While it makes sense, it wasn’t until after Johnson and Eisenhower died that science discovered that dietary fat contributes only a small amount to blood lipid levels. The idea was popularized from the seminal work of Ancel Keys. We did not have statins then, and we were not yet to the point of illucidating that dietary cholesterol was a minimal contributor to blood cholesterol but saturated fat was a major one.
But in spite of evidence to the contrary, once a popular notion is in the press, it stays there. Which brings us to President Clinton. The president enjoyed his burgers, and when he had his heart attack he began to examine the notion that plant based diets would reverse heart disease. His disease arteries bypassed, he turned to Dr. Dean Ornish. Ultimately, Clinton became a vegan. He has since liberalized his diet.
It has been years since Dean Ornish published his data showing a 3 per cent reduction in the plaques seen by coronary angiograms on a select group of patients who followed his Ornish diet and “lifestyle” plan. To be exact: the 28 patients who followed his plan had a 1.75% decrease in atherosclerotic plaque after one year and 3.1% decrease after five years. With the control group there was an increase of 2.3% in one year and 11.8% at five years.
No one has reproduced that data. No one. Still, from one old paper Dean Ornish has made a career; first being the anti-Atkins, and riding the anti-cholesterol, low-fat band wagon with the same religious fervor as Keyes did thirty years before. Ornish has since become the lead health-blogger for Huffington Post, has influenced Bill Clinton – turning him into a vegan, and is favorably mentioned by Dr. Oz.
The difficulty is this: science has caught up with him, and we know a lot more about how atherosclerotic plaques form. We know that dietary fats are far less important that what the body makes (often as a result of genetics) .
What Ornish and his crew call a landmark paper, had some issues:
(a) No one compares angiograms – a two-dimensional photograph of an artery – because they can be manipulated so easily and interpreted differently from one experienced radiologist or cardiologist to another. Depending on the angle you take the angiogram from, you can show a reduction in plaque by varying the recorder by a few degrees. Today intra-vascular ultrasound is the test of choice – this gives us a three dimensional view of the artery, from within the artery. The recent article in The New England Journal of Medicine, comparing lipid medications and their long-term effect on atherosclerotic plaque, is the most accurate measurement of plaque and its formation.
(b) We know about the science of lipids, plaque formation, and how we can manipulate those to provide a better answer for atherosclerosis that need not involve severe manipulations of a diet. For example, it appears that carrier proteins cause the damage to the arteries – and more carrier proteins are made in response to certain stimuli including saturated fat.
(c ) There were deep and troubling issues with the groups of patients serving as controls. For example, we do not know how many pack-years of smoking were in one group or the other. This is not a minor flaw, as science understands the highly inflammatory changes that are made with smoking as opposed to those made with hyperlipidemia.
(d) Lipid lowering drugs were used in some, and not others – however, the drugs today are far better, and more targeted than before.
To this day when most talk about saturated fat we are given “alternatives” like margarine, olive oil, oils from nuts, seeds, and the like. They are suppose to be better for us than “animal fat.” They are to an extent, but we have better ways of dealing with it.
We built pyramids – food pyramids, based on avoiding certain foods. We went out of our way to define the chemical nature of fats: polyunsaturated, monounsaturated, a trans-fats. We made charts so we could keep track of which fats were the “good fats,” so we could tell patients to eat these.
| Monounsaturated fat | Polyunsaturated fat |
| Olive oil | Corn oil, Grapeseed oil |
| Avocados | Fatty fish |
| Almonds, peanuts, macadamia nuts | Walnuts, sunflower seeds, flaxseed |
Then of course we had to tell people what was “bad” because it caused problems so we made tables like this:
| Saturated fat | Trans fat |
| Beef, lamb, pork | Margarine (stick form) |
| Ice cream | Fried foods (french fries, breading) |
| Milk, cream | Crackers, popcorn, chips |
| Lard | Shortening |
But wait – then we had to tell what to change in their diet so we made tables like this one:
| Less Healthy | Better Choice |
| Beef that is corn-fed | Beef that is grass-fed
Even better is salmon by ten times. Farm raised is better than wild. |
| Butter | Olive oil |
| Standard eggs | Eggs high in omega-3 fatty acids |
| Ice cream | Frozen yogurt |
| Milk | Fat-free milk, soy milk, almond milk |
| Shortening, lard | Grape seed oil, canola oil, vegetable oil |
Did I mention we were wrong?
In science, we make a hypothesis – then test the hypothesis – then based on our findings, we refine things, test again, and somewhere we develop a theory that explains the nature of things. In this case – food.
When the USDA and Europeans looked at the data to make recommendations about fat, they cherry-picked the data about saturated fats. Meaning, despite studies showing that saturated fat did not increase heart disease. We now know that saturated fats increase blood cholesterol and that to decrease risk you must have dietary saturated fat at less than 9 percent of fat intake. Although we prefer less than five per cent.
guidelines and recommendations that were based not on critical thinking, but the bias of the committee members.
Remember: in those days, everyone had the thought that the fat laden arteries of people with coronary artery disease came from butter, animal fat, and the like.
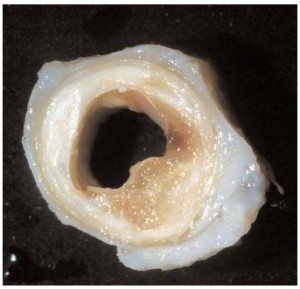
Heart artery plaque- low fat diet doesn’t prevent this
What do we do?
It turns out that saturated fat is still problematic bad for a person,
Still, the ideas of eating “healthy” for many people means avoiding red meat, avoiding saturated fats. We do have better methods of controlling LDL.
How We Live:
Which brings us to one simple fact: how we live is more important than how when we die- especially if the quality of life is less than satisfying. I doubt Eisenhower enjoyed his last days as much as Lyndon Johnson.
But let me bring one simple point: learn to cook. Appreciate fresh food. Yes, you can live on processed food but you cannot thrive.
REFERENCES:
In 2003, a meta-analysis of over 50 trials was published examining the relationship of dietary fat to serum cholesterol levels (Mensink RP, Zock PL, Kester AD, Katan MB. Effects of dietary fatty acids and carbohydrates on the ratio of serum total to HDL cholesterol and on serumlipids and apolipoproteins: a meta-analysis of 60 controlled trials. Am J Clin Nutr 2003;77:1146–55.). The conclusion was that saturated fat increases the levels of low-density lipoprotein (LDL) and high-density lipoprotein (HDL) but without changing the ratio of total to the HDL cholesterol. They concluded that using cholesterol alone as a marker of risk was unreliable. This was because if you replace the saturated fat with carbohydrates or tropical oils if you examine the effects on HDL and apolipoprotein B. They concluded that “… we can never be sure what such fats and oils do to coronary artery disease risk.” To translate that from doctor-scientist language: we can improve some laboratory markers, but really not by any mechanism that makes a difference from what we know.
While a systematic review of randomized trials showed that when saturated fats are replaced by polyunsaturated fats there is a reduction in the laboratory marker for risk of heart disease, there was no association with mortality from heart disease. To emphasize this: the laboratory values of the patients studied improved, but their mortality didn’t. The review also showed that monounsaturated fat intake significantly increased cardiac events, but no effect from the intake of saturated or polyunsaturated fat. Let me emphasize that: Monounsaturated fats, by at least one study, not only didn’t improve issues with the heart- the patients in that study did worse.
When examining other prospective studies about the risk of saturated fat and cardiovascular disease, there has been a consistent lack of an association between fat intake and heart disease, stroke, or total cardiac events.
Cohort studies show that by replacement of saturated fats with unsaturated fats, or carbohydrates – and examining the hazard ratios for heart attacks and deaths from heart disease were as follows: 0.87 for polyunsaturated fat, 1.19 for monounsaturated fat, and 1.07 for carbohydrates. For those not familiar with statistics, these are essentially no difference, and if these small statistical numbers are accepted than polyunsaturated fat shows an alarming trend. So here is a study that indicates (with as much precision as most studies these days) that polyunsaturated fats are worse for you than saturated fats.
There is a difference between protection against what we define as risk of heart disease and death from heart disease. Risk reduction means that we lower the laboratory values of factors we associate with risk – but the end point is death. In a meta-analysis published in 2010 (Ramsden CE, Hibbeln JR, Majchrzak SF, Davis JM. N-6 fatty acid-specific and mixed polyunsaturated dietary interventions have different effects on CHD risk: a meta-analysis of randomised controlled trials. Br J Nutr 2010;104:1586–600.) examined seven different trials, they found that there was a risk reduction but no change in mortality. Another study (Skeaff CM, Miller J. Dietary fat and coronary heart disease: summary of evidence from prospective cohort and randomized controlled trials. Ann Nutr Metab 2009;55:173–201. ) had eight trials found “There is probably no direct relation between total fat intake and risk of CHD (heart disease).”
The advice of the USDA is reflected in places like WebMD, recounted in public service commercials, and recited as gospel by health care workers everywhere. Giving false impressions about what an appropriate diet is.
