Lap-Band: some centers should not do them:
When a bariatric group consistently gets poor results from a procedure they should not do that procedure. In this case, a number of bariatric surgeons have had poor results with patients who underwent the Lap-Band. Those groups often blame the Lap-Band as the problem- but with the band it isn’t the procedure, it is how the surgeons take care of their patients after they have the operation.The results from those centers are in stark contrast to Lap-Band surgeons who prefer the band, who have great results with their patients, who see their patients often.
There is an essential difference between weight loss surgeons: those who think the surgery should do everything, and those who think surgery is a tool and we should teach lifestyle changes
One key to teaching patients about how to take care of the band is to enforce that the band is NOT ABOUT RESTRICTION. The band does not, and should not restrict food. Instead the band should allow food to go freely past the band. If food stays above the band too long, it will become uncomfortable. Ultimately this causes stretch with the stomach on top of the band and begins a process of dilation and as the stomach above the band dilates, it begins to pull stomach from below up to the band.
Once this happens there is what is called a band slip. It is at this stage that some surgeons mistakenly believe it is the band that has failed, and then remove the band and convert patients to a gastric sleeve. Converting to a sleeve in these circumstances comes with a 5.5% leak rate– meaning, it is far more deadly to convert these patients to a sleeve if they have a dilated stomach.
There are two better alternatives, however. One alternative is to remove all the fluid from the band and place the patient on a strict liquid diet for a week. Recheck an x-ray and often times the band will be back in a normal position. During this time the patient needs to be educated about how to use the band, and not use the band. Behaviors that cause slips include: relying on the band to feel full, eating too fast, getting foods stuck too often. The worst way a patient can use the band is to rely on the band to make them feel full. If they do this, they will cause the stomach above the band to stretch, as it stretches stomach is pulled from below the band to above the band and result in a slip or dilation of the upper pouch — early on giving symptoms of reflux and heartburn.
The second alternative is a surgery to unbuckle the band. This takes the pressure off the upper stomach. There is scar tissue from where the band and the stomach were and that scar tissue must be opened up. This is a quick operation, takes about ten minutes, and allows the person who could not eat or drink to immediately be able to. Then, in two months the patient has a choice to have the band re-buckled, leave it alone, or if they wish to go to another weight loss operation there is much less risk of a leak. We have done over 20 patients with unbuckling the band, and later repositioning it. All with great results, no morbidity or mortality in that group.
The key, however, is having a band surgeon who knows how to take care of the band, and not a surgeon who is quick to abandon the band and not wish to teach the patient how to use it.
Gastric Sleeves can Stretch over time:
The problem with the gastric sleeve: it can stretch over time. Having done hundreds of sleeves, after four or five years we see that some of them stretch, and sometimes will stretch back to the size of a normal stomach. That same behavior that caused the stretching of a pouch above a Lap-Band will ultimately lead to stretching of the sleeve — then the patient is faced with another choice. A number of my patients who underwent duodenal switch, or gastric sleeve, years ago and had their stomachs stretch, have had the lap-band placed over them, with great results – again, being taught that the band and the sleeve are tools, and not tools to make you feel full.
So it is important to know that lifestyle is key to gastric sleeve as well as to all weight loss operations.
We love the gastric sleeve as an operation, and were the first to do it as a stand-alone operation in Arizona. We think it might be the best choice for those who really want help to “stop” eating. It is also a great choice for some who travel a lot and don’t wish to worry about having a device in them.
Great results are not from the procedure: it is from teaching patients about aftercare and lifestyle.
That is the key to having success with the least invasive operation – and after 20 years of doing all the weight loss operations – the key to success in all operations is teaching patients a new lifestyle. Not that there are not complications with surgery- as there are with any operation – but it is quite clear: there is a huge difference in the results of those who have a band done from a center where they specialize in the band and the aftercare of the patient, and those centers where band is an afterthought.
Not everyone should be doing the band: that is clear from the literature of those centers that have removed bands.
Still, the Lap-Band is the most researched weight loss surgery to this day. In part because it is the least invasive, in part because it does not remove stomach, and in part because it is the only surgery that is approved for patients who have less weight to loose- meaning it is much safer.
If you had your band and find that you are having issues, but the place that did your band wants it removed – get a second opinion from a surgeon who does a lot of bands. Go to lapband.com and see the surgeons who are listed there. At one time your surgeon may have been listed there, but the results may have them removed from that list.

The lap band is placed at the top of the stomach – here is a diagram of the band placed in its normal position
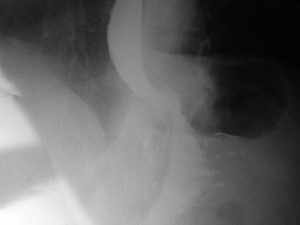
- This is a normal band x-ray. The band is the faint outline in a 8oclock to 2 oclock position, there is normal contrast going through it.
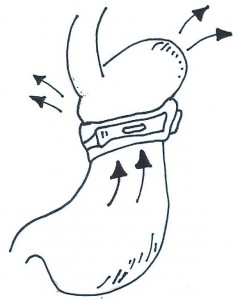
- Relying on food to go slowly through the band, and having the band too tight means food stays above the band. Some people say this makes them “feel full” but it ends up causing a band slip

- Once there is enough stomach above the band, it flops over the band – like a muffin top. At this point patients experience heartburn, reflux, sometimes night cough
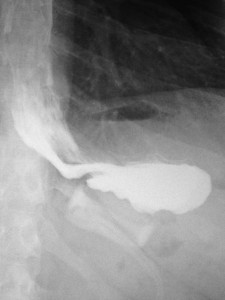
- The x-ray shows the band now in a 10 oclock to 4 oclock position, with the stomach pulled above the band, and the muffin top
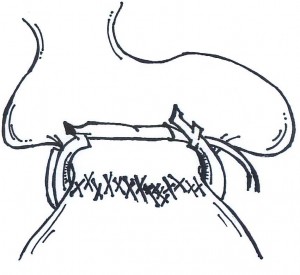
- Here is a diagram of an unbuckled band. Below the band, on the stomach is the scar tissue which must be lysed (or cut) to allow healing
