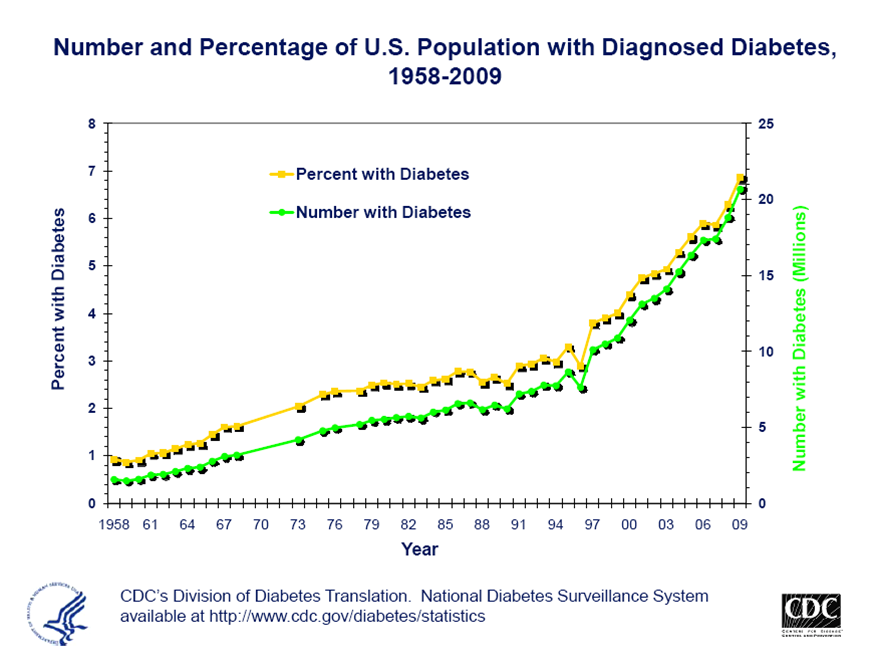
 There is no “glimmer of hope” in the trends of diabetes in the United States showing that about 14% of the population has diabetes. What is more concerning is half of the U.S. population has either diabetes or pre-diabetes. Diabetes is a major cause of illness and death in the U.S. Costs about 245 billion in 2012 due to healthcare costs and lost productivity.
There is no “glimmer of hope” in the trends of diabetes in the United States showing that about 14% of the population has diabetes. What is more concerning is half of the U.S. population has either diabetes or pre-diabetes. Diabetes is a major cause of illness and death in the U.S. Costs about 245 billion in 2012 due to healthcare costs and lost productivity.
Diabetes is the major cause of blindness, kidney failure, heart disease, strokes, amputations, and the sixth most common cause of death in the United States.
When looking at the data from 25 years ago compared to today diabetes increased in every age, gender, and ethnic group – including every educational level and every income level. In short, diabetes does not discriminate.
What is more concerning is half the US has either pre-diabetes or diabetes.
Diabetes in the United States was stable in the 1960’s to the 1980’s. Then there was a rapid increase in diabetes from the 1988 to 2008. What did not increase was undiagnosed diabetes. Decrease in undiagnosed diabetes secondary to better screening. Those with lower access to healthcare have not had such improvements.
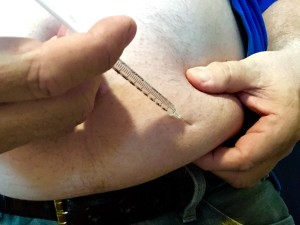
Diabetes and Pre-Diabetes affect half the US population
Preventing Diabetic Issues
Diagnosis of diabetes and treatment of the blood sugar remain the cornerstone of preventing hospitalizations for its sequel. Southcentral Foundation’s Nuka System of Healthcare, has shown that while diabetes has increased, the development of a relationship between the primary care provider and the patient reduced hospitalizations and emergency room visits for diabetes.
Intensive lifestyle intervention showed that dropping weight by 7% resulted in a 58% lower incidence of diabetes than even those who received Metformin (the first line drug used by most for diabetes).
However, when it comes to obesity with diabetes, there is only one effective and cost efficient tool. That is weight loss surgery.
The Only Effective Treatment For Diabetes and Obesity
The upward trends of diabetes and pre-diabetes mirror the trends in obesity.
For those who have obesity there is only one treatment effective against diabetes and obesity, and that is weight loss surgery.
It is not only effective- but it is the most cost-effective. Below from the Australian study:
Mean 2-year intervention costs per patient were 13,400 AUD for surgical therapy and 3,400 AUD for conventional therapy, with laparoscopic adjustable gastric band (LAGB) surgery accounting for 85% of the difference. Outpatient medical consultation costs were three times higher for surgical patients, whereas medication costs were 1.5 times higher for conventional patients. The cost differences were primarily in the first 6 months of the trial. Relative to conventional therapy, the incremental cost-effectiveness ratio for surgical therapy was 16,600 AUD per case of diabetes remitted (currency exchange: 1 AUD = 0.74 USD).
CONCLUSIONS
Surgical therapy appears to be a cost-effective option for managing type 2 diabetes in class I and II obese patients.

The lap band is placed at the top of the stomach – here is a diagram of the band placed in its normal position
In all of the treatments that have been listed, only bariatric surgery has been found, in good studies, to reverse or slow diabetes, and reduce obesity. First shown with the Lap-Band, and then later confirmed with the RNY-gastric bypass and the now popular gastric sleeve – diabetes control is made better or diabetes goes into remission.
Success in bariatric surgery requires the patients to adopt a lifestyle that involves less refined sugars, less refined carbohydrates.
REFERENCES:
Menke A, Casagrande S, Geiss L, Cowie CC. Prevalence of and trends in diabetes among adults in the United States, 1988-2012. JAMA. doi:10.1001/jama.2015.10029.
REDUCTION IN THE INCIDENCE OF TYPE 2 DIABETES WITH LIFESTYLE INTERVENTION OR METFORMIN
Diabetes Prevention Program Research Group
N Engl J Med. Author manuscript; available in PMC 2006 February 17.
Published in final edited form as: N Engl J Med. 2002 February 7; 346(6): 393–403. doi: 10.1056/NEJMoa012512
PMCID: PMC1370926
Bariatric surgery: an IDF statement for obese Type 2 diabetes
J B Dixon, P Zimmet, K G Alberti, F Rubino, on behalf of the International Diabetes Federation Taskforce on Epidemiology and Prevention
Diabet Med. 2011 June; 28(6): 628–642. doi: 10.1111/j.1464-5491.2011.03306.x
PMCID: PMC3123702
Effects of Gastric Bypass Surgery in Patients With Type 2 Diabetes and Only Mild Obesity
Ricardo V. Cohen, Jose C. Pinheiro, Carlos A. Schiavon, João E. Salles, Bernardo L. Wajchenberg, David E. Cummings
Diabetes Care. 2012 July; 35(7): 1420–1428. Published online 2012 June 12. doi: 10.2337/dc11-2289
PMCID: PMC3379595
Cost-Efficacy of Surgically Induced Weight Loss for the Management of Type 2 Diabetes: A randomized controlled trial
Catherine L. Keating, John B. Dixon, Marjory L. Moodie, Anna Peeters, Julie Playfair, Paul E. O’Brien
Diabetes Care. 2009 April; 32(4): 580–584. Published online 2009 January 26. doi: 10.2337/dc08-1748
PMCID: PMC2660476
