Wearable Technology
You probably have one: an apple watch, maybe a Fitbit – or perhaps last year’s darling the Nike Fuel. If you are more sophisticated you might have Garman’s Epix or some other wearable.
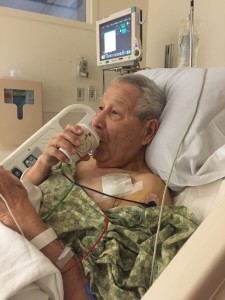
They are the future of medicine, and things that we, as physicians, wish people could wear and we could have access to. Never was this a better example than with my dad.
“Your Father is non-responsive and the paramedics are here.”
Those are not words you want to hear from the assisted living center where your 91-year-old father is living. Talking to the paramedics, he did get some fluid and was talking to them, no sign of a stroke but was on his way to the hospital “Big Prov “ they called it (the major Providence Hospital in Portland).
I traveled the 11 miles in record time, beating the ambulance that had my dad by ten long minutes. I didn’t tell the ER check in person that I was a doctor, just told them who I was waiting for and they knew he was coming.
When they let me back into the ER area my dad was settled in, joking with the nurses, and had already had his blood drawn and his pacemaker had been “queried.”
Turns out my father became “vasovagal” after straining to have a bowel movement. He then stood up and passed out. The assisted living folks called 911.
Because the ER physicians could look back over his heart rhythm on the pacemaker they could see he did not have a cardiac rhythm disturbance, didn’t have a heart attack. Dad just a simple bit of light headedness because he strained too hard, was a bit dehydrated, and stood up too soon.
Had my dad not had a pacemaker they would have admitted him to a heart monitoring unit for the night, spent more time and money evaluating him, and released him in a couple of days.
But my dad had the ultimate wearable technology. His pacemaker. They could look back and see every heartbeat, if it was normal or not, and they could tell his heart was fine, and he didn’t even need to have a pace from the machine.
Today’s wearable technology has some of this capability, and yet is hindered because of some of the FDA requirements. Tim Cook, CEO of Apple, noted that they may make some wearable technology but it will be a different line than the apple watch. Before the watch originally came out there was talk that it would have other sensors built in, but that would move it from a “wellness” tracker to a medical device.
Innovation stifled by regulations
Opening up innovation could help physicians and patients have technology that is less invasive and expensive than the pacemaker. A wearable would be able to tell a physician like me if a patient’s heart rate goes up, if they are active or sitting, if they are having an issue and to look at data over time. The technology to do this is available but sitting on the shelf.
Surgeons could see the postoperative patients on-line; instead of having them travel to the office. The surgeon could answer their questions, and based on the information could ask them to come in, or – for the vast majority – re-assure them they are doing just fine. The pediatrician could look at the child’s respiratory rate and see if they responded to a home treatment, or if they need to come into the office or go to the hospital.
For some patients it would save their lives: that bit of heartburn you felt might be a heart attack and someone could notify you to come into the hospital and have things taken care of. It could tell if your asthma was getting out of control and you need to change medicines, or take medicines. It might tell if you were in danger from having had a stroke and are not moving and they need to send help to you.
The right helmet on an NFL player will tell the staff that the hit was over 5 G’s and the player needs to come in and be out for the game or the week, or the year.
Even today right wearable will tell you that you are over-training and you need to back off so you don’t injure yourself. The Epix will do that.
I have seen the future. It saved my dad a hospitalization, and given the bad things that can happen in a hospital (a hospital acquired pneumonia, a MRSA infection, the wrong drug given accidentally) – it may have saved his life. In this case, it allowed him to go home on Thanksgiving evening to see his wife of 68 years, and reassure her that he was OK.
On the shelves are some great technology that will save patient’s lives, but mostly they are expensive “wellness trackers.”