Eastern Medicine – practicing with an ancient license
 I am reading through Twitter about how Gwyneth Paltrow and her “Goop” brand is trying to sell an expensive lifestyle with pseudoscience. When called out by legitimate physicians, like Jennifer Gunter, or Steven Novella, they counter with how they integrate “Eastern” into “Western Medicine.” The Goop website is filled with misinformation: tomatoes are toxic, lectins cause obesity, EBV causes thyroid disease, bras cause breast cancer, and their $66 jade egg, when placed in a vagina will improve pelvic wall function and enhance their orgasms, colonics are good, you need to detox from heavy metals, and parasites are found in 66% of people and they can be removed by drinking goat’s milk. GOOP has now pulled the “Eastern Medicine” card – meaning, they don’t want to talk legitimate science, they want to find reason to peddle their expensive snake oil to latte sipping English majors who eschewed science courses and critical thinking.
I am reading through Twitter about how Gwyneth Paltrow and her “Goop” brand is trying to sell an expensive lifestyle with pseudoscience. When called out by legitimate physicians, like Jennifer Gunter, or Steven Novella, they counter with how they integrate “Eastern” into “Western Medicine.” The Goop website is filled with misinformation: tomatoes are toxic, lectins cause obesity, EBV causes thyroid disease, bras cause breast cancer, and their $66 jade egg, when placed in a vagina will improve pelvic wall function and enhance their orgasms, colonics are good, you need to detox from heavy metals, and parasites are found in 66% of people and they can be removed by drinking goat’s milk. GOOP has now pulled the “Eastern Medicine” card – meaning, they don’t want to talk legitimate science, they want to find reason to peddle their expensive snake oil to latte sipping English majors who eschewed science courses and critical thinking.
“And speaking of doctors, we are drawn to physicians who are interested in both Western and Eastern modalities and incorporate the best from both, as they generally believe that while traditional medicine can be really good at saving lives, functional medicine is more adept at tackling issues that are chronic.” – from their website answering criticism.
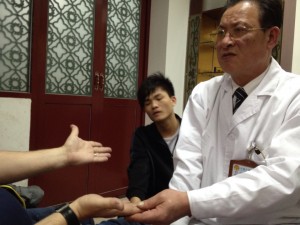
A doctor of Chinese medicine (in China), diagnosing me. Apparently I needed to pay him to do some “energy therapy” to cure my inflammation.
Besides being unadulterated bullshit, the implication is there is a body of knowledge, or “Eastern medicine,” that has something to offer for treatments and cures of modern disease that we physicians in the West are clueless about. This is a logical fallacy, “appeal to antiquity.” This fallacy goes like this, “they have been doing this for thousands of years so it must be right.” Translated – goop.com is selling old bullshit to the uninformed.
Goop, like all who appeal to antiquity, want to make you feel as if they are enlightened to integrate the Eastern and Western medicines. That they, and not Western Medicine, question authority and seek truth. But it is science, that is, Western Medicine, that questions beliefs, that has relentlessly tested “old remedies.”
It is science that has shown most of the nonsensical treatments sold on GOOP are ineffective. Western Medicine is not forever locked as if all knowledge were discovered by the ancient ones, and we need only return to those ancient traditions. Goop, like Eastern Medicine or pseudoscientists are not open minded. Like many pseudoscientists they have one job- to sell you their nonsense and convince you that they have some secret knowledge that “Western” medicine has lost. Pseudoscience loves to play the Galileo Gambit.
The Galileo gambit : the world rejected Galileo’s thought, just like they reject me. Implication is that the pseudoscientist, like Galileo, is right. Unlike the pseudoscientists, Galileo supported his beliefs with evidence.
I have an acquaintance who received his MD degree in Eastern medicine – instead of taking the usual four years of medical school it took him six months (online degree from India). Thankfully no state would grant him a license to practice medicine. The use of the term “Eastern medicine ” is another way that some people want to practice medicine and ignore the rigors of a “Western” education. Western medicine requires you to have a basic understanding of science, the scientific method as well as an in depth knowledge of anatomy, physiology, and biochemistry.
Medicine, and discoveries about treatments of diseases, are not discovered and hidden. There are no hidden manuscripts that only Chinese acupuncturists, or “functional” or “integrative” physicians know about. Worldwide medical journal articles and texts are translated immediately. Important medical breakthroughs across the world are instantly transmitted to our iPads or other electronic readers. It is ironic that some people make an assumption that “Eastern medicine” is a big secret, and the food cons will try to convince you that they have discovered its hidden secrets and can cure you through food. Sadly, people who infest goop.com are not having a legitimate conversation about food, just doing the food con – giving those of us in the field of Culinary Medicine fits.
Culinary Medicine is a legitimate field, there is a lot of great journal articles in Western Journals, with testing on millions of people with data (not millions of anecdotes). We know that food can serve as a great tool to help with medicine, but it is a disciplined field, a part of “Western Medicine.” If I prescribe a low-sodium DASH diet I know what to expect, because it has been tested and retested, and we know the results. I would never prescribe goat’s milk to get rid of parasites. Nor would I tell people to avoid wheat if they have thyroid disease. Sadly Goop.com doesn’t go with doctors who practice Culinary Medicine, instead they have a group of people offering nutritional advice with a kernel of truth and a mountain of bs. Of course, they want to sell you products: like Dr. Gundy’s “Vital Red” – for which there is no good evidence. Or Gopp.com $70 a month vitamins (you can buy equivalent quantity and quality of vitamins from Costco for about $10 a month).
There is no secret in Japan or China about how to treat or cure disease that Western Medicine doesn’t immediately hear about and test. It is comforting to think there might be some ancient wisdom, though, things that didn’t get translated. Let me take you to the mid 1800s, at a time when “Eastern medicine” had developed with no influence from the West.
Why Japan Has Western Medicine
There was a doctor, Takaki Kanehiro, from the region of Satsuma in Japan. He was classically trained in Japanese (Eastern) medicine. Early in his career as a physician, he was laughed at when a doctor from Nagasaki said, “There are no doctors worth mentioning in Satsuma.” The system of medical education was an apprenticeship in the venerable Eastern medicine. Much of it learning of herbs and potions in ancient texts passed on from one generation to another.

In the background the modern St Thomas Hospital
Takaki’s sense of embarrassment led to him seeking to further his knowledge as a physician, and ultimately to study of Western medicine, under the British physician William Wills in 1870, who was living in Japan. Later, Takaki travelled to London, and St. Thomas’s Hospital (across the river from British Parliament), where he stayed for five years and even won St Thomas’s highest awards for his work. He learned from Western medicine not just a new apprenticeship with the techniques of the day, but a method of thought—the scientific method.
Takaki Kanehiro is revered because he helped to found and foster what has become medical education in Japan, translating from what was a traditional Eastern style to the scientific method that provided Japan with the tools for the study of disease. It was because of learning the scientific method of thought that he hypothesized that beriberi was a nutritional deficiency. Thus it turns out that Western medicine cured a disease in Japan.
How Western Medicine Cured Beriberi – a disease that Eastern medicine couldn’t

Kanehiro not only revolutionized medical education in Japan, adopting Western Medicine, he showed how the scientific method would cure beri beri.
In the latter half of the eighteenth century, beriberi was widespread throughout Southeast Asia, especially in Japan, as well as China, Indonesia, Java, and the Philippines. A little over one third of all illness in the Japanese navy was from beriberi. Beriberi is a disease caused from a deficiency of vitamin B1 (thiamine). Without thiamine, the body cannot utilize the energy from carbohydrates, fat, and protein. Symptoms include weight loss, weakness, pain in the limbs, impaired sensory perception, emotional disturbances, irregular heart rate, and swelling of the lower extremities (edema). It might start with difficulty walking, followed by tingling or loss of sensation, mental confusion, pain, and can progress on to heart problems and death. The confusing complex of symptoms all comes from the deficiency of just one vitamin.
Much like James Lind did with scurvy, Takaki looked at various theories of the cause of beriberi—clothing, living quarters, and even the temperature of the places the ships went. He noted that the officers of the ship rarely contracted beriberi and had access to more variety of food. In contrast sailors and the prisoners on the ships, had more beriberi and tended to eat primarily polished white rice, and had beriberi. Takaki also noted that when ships were in port, many of the sailors with beriberi recovered. His belief that diet was a component of beriberi had to be tested.
His experiment was set up with a ship that was given increased provisions of bread, meat, and vegetables. The ship followed the route of a control ship that had the usual provisions, where most of the crew would eat white rice. The control ship had 169 cases of beriberi among the 370-member crew, with twenty-five deaths. In the test ship, there were no cases of beriberi. This prompted reforms to increase the food provisions among the Japanese Navy. In 1882, when Takaki had started looking at beriberi there were an average of 404 cases of beriberi for every one thousand sailors, and after his reforms were implemented in 1886 there was less than one case per thousand.
Fifteen years after Takaki published his success in treating beriberi, the world had still not been convinced that beriberi was caused by a nutrient deficiency. In those days, iPads were not readily available, and few in Europe read Japanese medical journals – in part because their “Eastern” medicine had proven itself unhelpful. On the Dutch colony of Java, a physician named Dr. Christiaan Eijkman was assigned to find the “microbe” associated with beriberi. Eijkman observed that chickens fed white, polished rice developed classic beriberi. When Eijkman fed unprocessed rice to chickens, the chickens didn’t get beriberi, even when inoculated with the “germs” from chickens that had beriberi.
In 1901, Eijkmann interpreted beriberi as a deficiency syndrome. For his work he was awarded the Nobel Prize in medicine in 1929. Takaki had died in 1920, nine years before the prize was awarded; the Nobel Prize is never given posthumously.
Eastern medicine didn’t cure beriberi, but someone who was classically trained in the west did. Takaki didn’t “integrate” his training in “Eastern” medicine – he tossed that false erudition as should we all.
